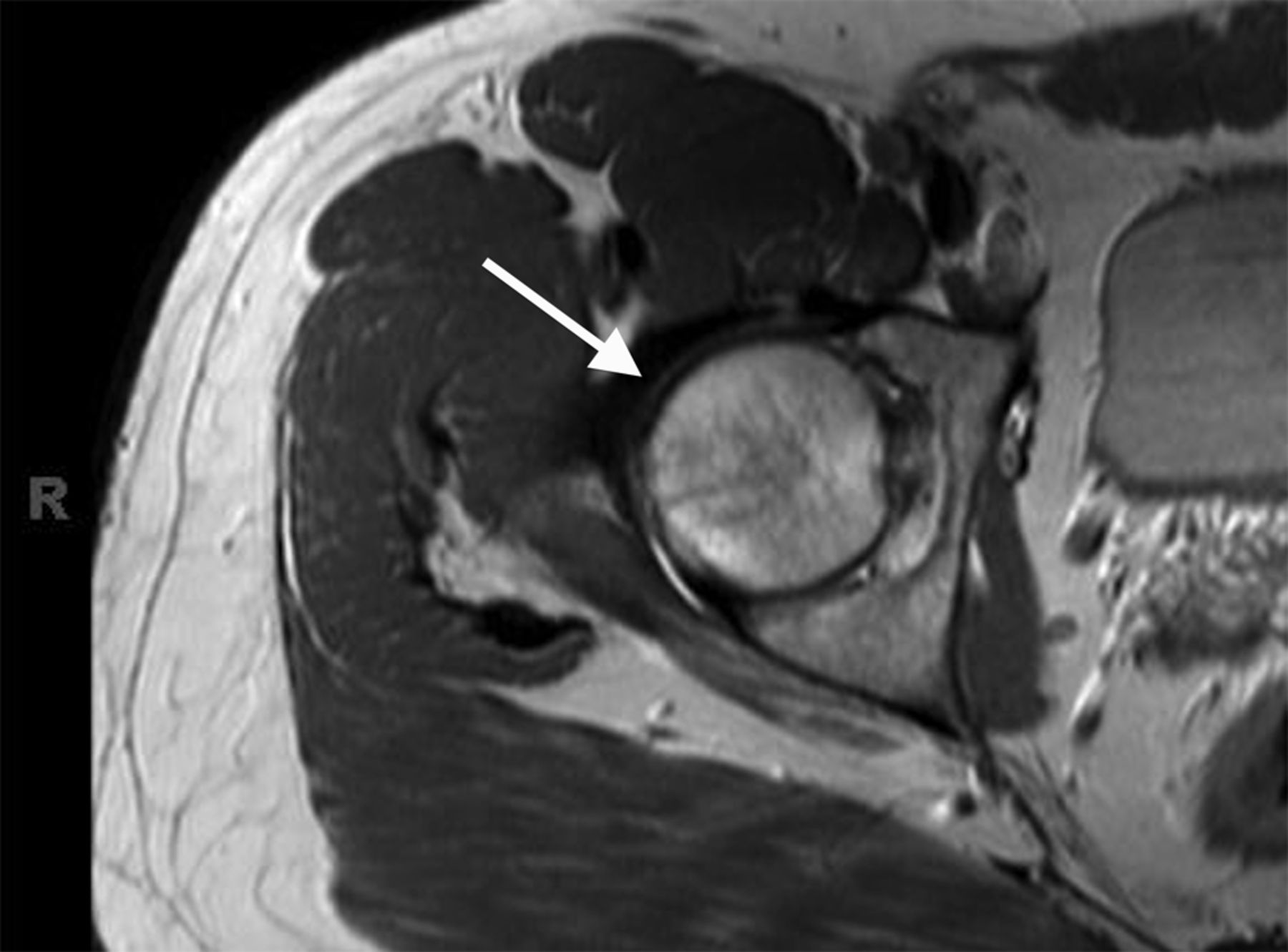
Although by the time the double line sign is visible, this is very late in the disease process. On T2-weighted images, there may be a bright signal line that parallels the dark line, which is referred to as the “double line sign,” which has worked its way into the lexicon of classical findings in radiology ( Figure 17-1C). The classic findings of AVN on MRI is a subchondral area of low T1 signal intensity, which is outlined by a dark T1 line ( Figure 17-1B). The dark and bright lines parallel each other giving rise to the “double line sign.” There is marrow edema in the femoral heads, more significant on the left side. Coronal STIR image shows both T2 dark and T2 bright serpentine lines in the femoral heads. Note that the AVN of the right hip is very subtle on the radiograph, but clearly visible on the MRI. ( B) Coronal T1-weighted MRI shows T1 dark serpentine lines in the femoral head, which extend to the subchondral surface. There is faint sclerosis without collapse of the right femoral head. ( A) Radiograph of woman with SLE shows flattening, collapse, and sclerosis of the left femoral head from AVN. Early AVN on MRI may just manifest itself as marrow edema.įigure 17-1. Early radiographic changes are seen as subtle osteopenia followed by sclerosis of the femoral head and then loss of normal contour ( Figure 17-1A–C). 1, 2 Table 17-1 lists common causes of AVN.ĪVN may initially be occult on radiographs, whereas its early stages may be visible on MRI. In trauma, the culprit can be disruption in the blood supply in lupus, the etiology may be due to vasculitis and in steroid use the etiology may be due to hypertrophy of fat cells leading to venous compression and then infarction. As with many other conditions, the true pathogenesis of AVN varies with etiology. There is a long list of conditions that predispose to AVN some of the more common ones are steroid use, alcoholism, sickle cell disease, lupus, and trauma. In the end, associated conditions like sacral fractures and some basic concepts of pubalgia or “sports hernias” are discussed briefly.ĪVN is a crippling process that can lead to collapse of the femoral head and the onset of disabling osteoarthritis. This is becoming a more common diagnosis as knowledge of it spreads and the population becomes more physically active at a younger age. Interested readers are referred to the references at the end of the chapter for further studies.ĪVN is discussed first, followed by less common conditions, and then basic concepts of femoroacetabular impingement syndrome are discussed. In this chapter, we provide a brief introduction of the hip pathologies one that is most likely to seen and then describe some relatively less common conditions. If AVN is a possible diagnosis but the MRI is equivocal, we suggest the referring physician put the patient on restricted weight bearing and repeat the MRI study in a month. In case of hip arthrograms, sequences are tailored to assess for labral pathology. Sagittal sequences are added to assess the musculature and look for what, if any, part of the weight-bearing surface is affected. T2-weighted fat-suppressed sequences are useful in assessing for edema. Then we scan the affected hip in axial T1-weighted or proton density and fluid-sensitive sequences. It also helps in comparing common anatomical variants or clarifying imaging artifacts. This helps in conditions like avascular necrosis (AVN) that might be bilateral. We routinely perform coronal T1-weighted and short-tau inversion recovery (STIR) sequences of the pelvis that include both hips.

It might be a referred pain, but it alerts the radiologist and the referring physician to the possibility of more ominous conditions like the beginning of an avascular hip necrosis. One should also remember that any unexplained hip pain without any apparent radiographic findings is an indication for MRI if the pain does not resolve within a week. Sometimes an injection of local anesthetics into the hip joint might be required to help diagnose the actual source of the patient’s pain.Īll imaging studies should begin with radiographs that help differentiate many benign conditions at the outset from what might appear to be very confusing on magnetic resonance imaging (MRI) studies. Moreover, the symptoms related to hip pathology can have myriad of manifestations ranging from focal pain to just a vague groin pain.


Since this joint transfers weight from the upper body to the lower limbs, it is subject to a range of problems resulting from faulty weight-bearing positions in normal individuals to problems caused by wear and tear in those who are athletically active. The hip joint is a ball and socket type of joint that is also the deepest joint in the body.
